Knowledge about topical steroid withdrawal, also called red skin syndrome and topical steroid addiction, has been partly driven by social media, with the hashtag ‘#TSW’ gathering over 1.1 billion views on TikTok4.
It describes a range of symptoms, some of which are already known side effects of topical corticosteroids, with the most common being redness and swelling that usually occur in people who have recently discontinued use4.
Topical steroid withdrawal is often confused with relapse of the original skin condition, yet the skin inflammation usually extends beyond the area treated with topical corticosteroids and develops in previously unaffected areas4.
It is more common after prolonged use of potent topical corticosteroids or after abrupt discontinuation. However, to date, it has not been reported with normal use, such as treating certain skin conditions for short periods or with short breaks in treatment over an extended period.5 It also seems to be most prevalent in women, accounting for 81% of cases.6
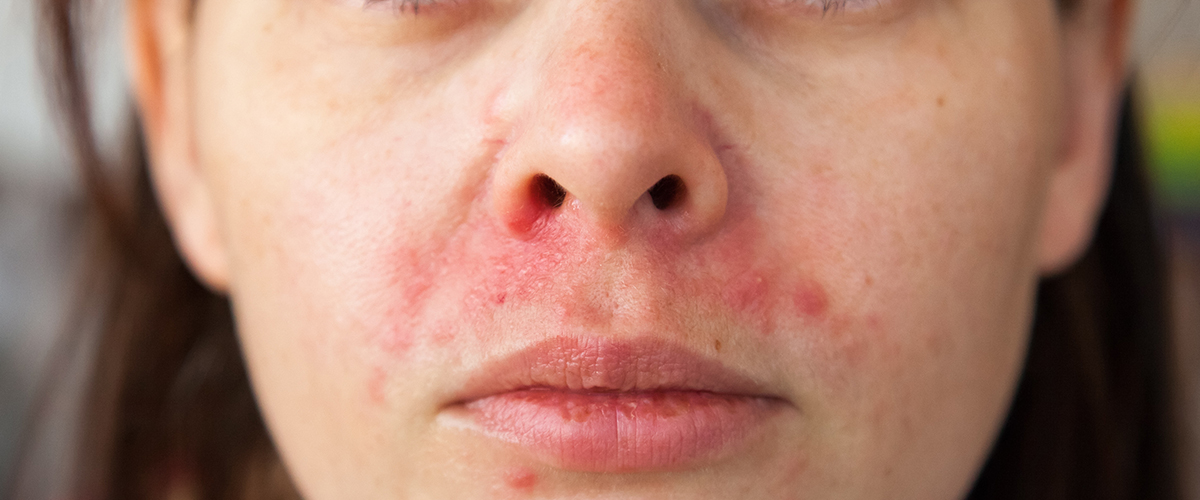
Some patients also report ‘elephant skin’, which is thickened skin with reduced elasticity; red sleeve sign, indicating redness of the limbs sparing the palms and soles; and headlight sign, referring to redness of the face while sparing the nose2,4.
It can be a frightening condition with a high psychological burden, as it can occur in sensitive areas such as the face and the genitalia, cause severe pain, and often disfiguring swelling7.
A common approach to topical steroid withdrawal recovery involves gradually tapering topical corticosteroid use and allowing the skin to heal naturally, although the duration, response, and symptoms can vary widely1.
For some, there may be four distinct stages once the steroid is stopped. It starts with burning and redness in the first few days, followed by dry, itchy skin. Then, as the skin begins to recover, there may be intermittent flares before reaching the final stage of recovery8.
Other management options include emollients, infection prevention, pain and itch management, and anxiety therapies2,9 Emollients can be applied multiple times daily, as needed during a flare, and used consistently over the long term to help maintain and support the skin barrier10.